Superior Vena Cava (SVC) Syndrome Nursing Notes, NCP & Management | NORCET & NCLEX
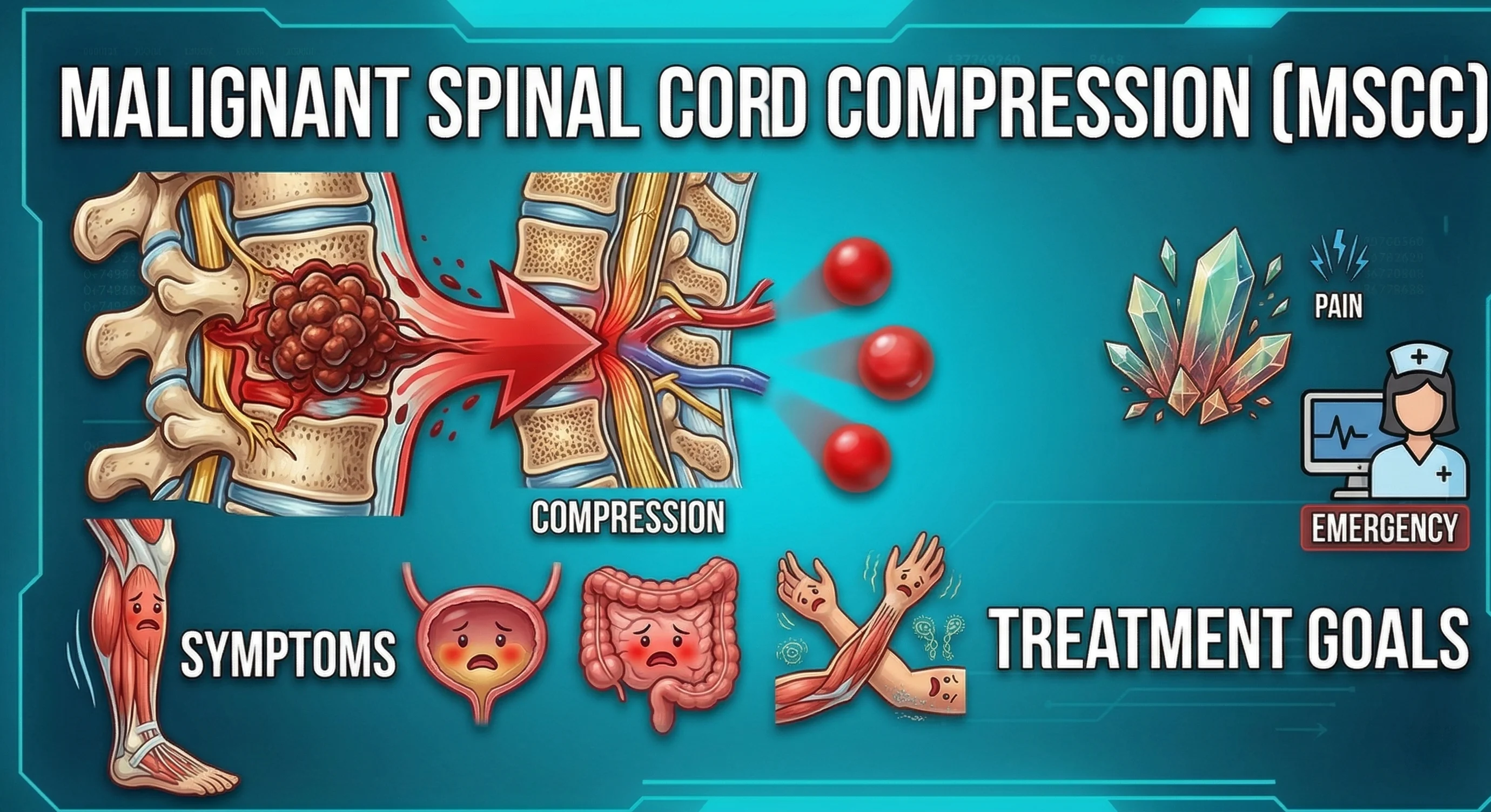
Superior Vena Cava (SVC) syndrome is a serious oncology emergency that requires immediate medical and nursing intervention. It occurs when the superior vena cava—the major vein that carries deoxygenated blood from the head, carries deoxygenated blood from the head, neck, upper chest, and arms to the heart—becomes compressed or blocked by a cancerous tumor.
For nursing students preparing for the NORCET and NCLEX exams, understanding the early warning signs of SVC syndrome and the precise nursing management is essential. Let's analyze the pathophysiology, clinical manifestations, and the complete Nursing Care Plan (NCP).
What Causes SVC Syndrome?
In oncology, SVCs are most commonly associated with cancers that develop in or spread to the upper chest. The main causes include:
• Lung Cancer (Small cell lung cancer is the most common cause)
• Non-Hodgkin lymphoma
• Tumor in the mediastinum
• Non-cancerous causes: thrombosis (blood clot) from a central venous catheter (CVC) or pacemaker wires.
Pathophysiology of SVC Syndrome :
Think of the superior vena cava as a massive highway that carries blood from the entire upper body to the heart.
1. A tumor grows in the chest that presses on this thin-walled vein.
2. This “highway” (vein) becomes blocked.
3. Blood pools in the head, neck, and upper limbs (venous stasis).
4. The fluid leaks into the surrounding tissues, causing severe swelling (edema) and compressing the airway.
Classic Signs & Symptoms: Early vs. Late
The primary responsibility of nursing is to detect SVC syndrome in a timely manner.
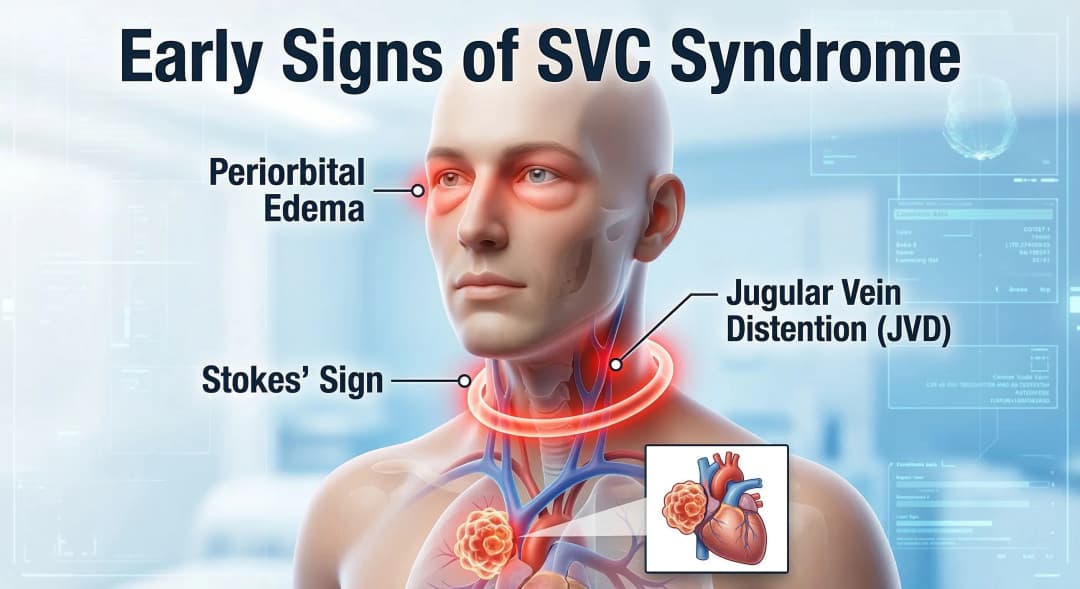
Early Warning Signs
• Facial swelling : especially around the eyes (periorbital edema), which is often most pronounced in the morning when the patient has been lying flat all night.
• Stokes' sign : the patient complains that the collar of his shirt feels completely tight around his neck.
• Veins in the neck (jugular veins), chest, and upper arms become prominent.
Late / Severe Signs
• Dyspnea (shortness of breath) and stridor (a high-pitched breath sound indicating an airway obstruction).
• Cyanosis of the face and upper body (turning blue)
• Altered mental status (caused by lack of oxygen in the brain)
• Dysphagia (difficulty swallowing)
Emergency Nursing Management & Interventions
When managing a patient with SVC syndrome, the focus is on reducing venous pressure in the upper body and keeping the airway open.
1. Patient Positioning (Most Important Nursing Action)
• Action: Elevate the head of the bed (HOB) to 30–45 degrees (semi-Fowler position).
• Rationale: It uses gravity to promote venous drainage from the head and neck, reducing facial swelling and making breathing easier. Never keep the patient completely flat (on their back).
2. Clinical Precautions
• Avoid the upper limbs: Do not take blood pressure or insert a needle into the veins (IV insertion/blood drawing) in the upper arms. Elevated venous pressure can cause excessive bleeding and prevent proper fluid drainage. If absolutely necessary and in accordance with hospital protocols, the lower limbs should be used.
• Avoid constriction: Remove any tight clothing, jewelry, or restrictive collars from the patient's neck and chest.
3. Medical & Pharmacological Support
• Oxygen therapy: Administer supplemental oxygen to relieve shortness of breath.
• Corticosteroids (e.g. Dexamethasone): Given to quickly reduce swelling and irritation around the tumor.
• Diuretics (e.g. Furosemide): Help remove excess fluid, although they are used cautiously to prevent the patient's overall blood pressure from dropping.
• Radiation/Chemotherapy: The definitive treatment to shrink a compressing tumor.
NANDA Nursing Care Plan for SVC Syndrome
Nursing Diagnosis | Nursing Interventions | Rationale |
Ineffective Breathing Pattern r/t tumor compression of the airway & chest | Lower the HOB to the semi-fowler or high-fowler position. Administer O₂ as prescribed. | The supine position maximizes lung expansion and also reduces fluid pressure on the upper airway. |
Altered Tissue Perfusion (Cardiopulmonary) r/t decreased venous return | Continuously monitor vital signs. Avoid placing blood pressure cuffs and IVs on the upper extremities. | Measuring blood pressure on weak or injured arms will give an incorrect result, and also poses a risk of tissue damage/bleeding. |
Anxiety r/t breathlessness and facial swelling | Stay with the patient, provide a calm environment, and explain all procedures. | Anxiety increases oxygen demand and respiratory rate, which worsens shortness of breath. |
Exam Corner: Check Your Knowledge
Q. A lung cancer patient reported that his shirt collar feels unusually tight first thing in the morning and his face appears swollen. What is the primary nursing action?
A) Lie the patient flat and elevate their legs
B) Elevate the head of the bed to 45 degrees
C) Prepare for an emergency tracheostomy
D) Insert a large-bore IV into the right arm
Answer: B – Elevating the head of the bed reduces venous stasis. Lying flat worsens the condition, and IV insertion in the upper extremities should be avoided.